Australia’s chief vaccine safety body has issued new advice affirming the safety of the AstraZeneca COVID-19 vaccine for people with a history of many blood clotting disorders.
But the Australian Technical Advisory Group on Immunisation also added two specific conditions to the list of health issues that should trigger a preference for the Pfizer vaccine.
In a joint statement released on Sunday, ATAGI and the Thrombosis and Haemostasis society of Australia and New Zealand (THANZ) said there were “no known markers for increased risk” from the vaccine.
A full list of the TGA’s latest advice on clotting related conditions and which vaccine to receive can be found below.

Specifically, Australians who have a family history of blood clots or incidences of deep vein thrombosis do not have a higher chance of vaccine-induced thrombotic thrombocytopenia – or TTS – occurring after receiving an AstraZeneca dose.
“TTS is a rare condition with a different mechanism to most other causes of thrombosis and/or thrombocytopenia,” ATAGI said in a statement.
“Among case reports, there are no known markers for increased risk for TTS.”
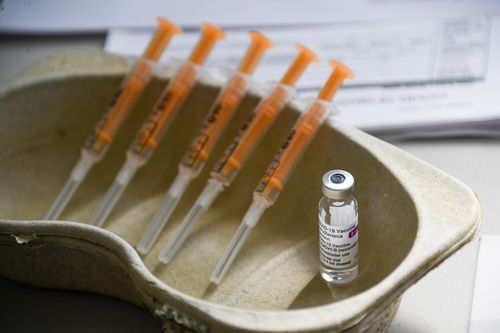
ATAGI was careful to point out that TTS “is a very rare potential complication” and that vaccination remains the best way to prevent severe illness from COVID-19.
“People who choose to delay vaccination until a vaccine other than AstraZeneca COVID-19 vaccine is available should be aware they may not be protected against COVID-19 for months,” the statement reads.
“The risk of potential outbreaks of COVID-19 is ever-present. The Australian population remains largely unimmunised and susceptible to COVID-19 risks.”
Currently, almost 3.6 million COVID-19 vaccines have been administered to Australians.
To date there have been 24 reports of blood clot cases in Australia relating to the AstraZeneca vaccine.
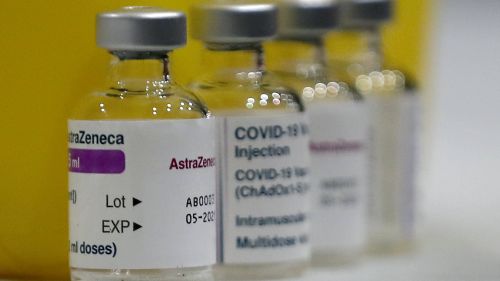
Two doses of AstraZeneca or Pfizer vaccine ‘highly effective’ against Indian strain: UK study
The study found that from April 5 to May 16, two doses of the Pfizer vaccine was 88 per cent effective against the strain and a similar dosage of the AstraZeneca vaccine was 60 per cent effective.
“The difference in effectiveness between the vaccines after two doses may be explained by the fact that rollout of second doses of AstraZeneca was later than for the Pfizer-BioNTech vaccine, and other data on antibody profiles show it takes longer to reach maximum effectiveness with the AstraZeneca vaccine,” the researchers write.
“As with other variants, even higher levels of effectiveness are expected against hospitalisation and death.”

The following groups of people can receive COVID-19 vaccine AstraZeneca:
- People with a past history of venous thromboembolism in typical sites, such as deep vein thrombosis or pulmonary embolism
- People with a predisposition to form blood clots, such as those with Factor V Leiden, or other non-immune thrombophilic disorders
- People with a family history of clots or clotting conditions
- People currently receiving anticoagulant medications
- People with a history of ischaemic heart disease or cerebrovascular accident
- People with a current or past history of thrombocytopenia.
Pfizer is preferred for anyone with:
- A past history of cerebral venous sinus thrombosis (CVST)
- A past history of heparin-induced thrombocytopenia (HIT)
- A past history of idiopathic splanchnic (mesenteric, portal and splenic) venous thrombosis
- Anti-phospholipid syndrome with thrombosis
- People with contraindications to COVID-19 Vaccine AstraZeneca
This content first appear on 9news

70918248
References:
Different Names For Steroids (Git.Fhlz.Top)
70918248
References:
what is roid (https://git.projet.parisnanterre.fr/perry49x938986)
Another side impact specific to women is clitoral enlargement, which can be everlasting.
This condition may cause discomfort and should affect sexual operate.
Women may also expertise a lower in breast measurement because the
body’s hormonal stability shifts. The increase in testosterone ranges can result in heightened aggression, irritability, and even despair in some circumstances.
Cambridgeresearch.eu.com is one of the prime
brands in the Europe and Center East and it’s
available within the market for more than 6 years and well-known & trusted
by the professional bodybuilders on the planet.
It can be necessary to steadily improve the dosage to
permit the body to adapt and minimize the risk of potential unwanted aspect effects.
Just to rapidly recap… anabolic steroids are synthetic substances much like the
male sex hormone testosterone. Although medical doctors do prescribe them to patients,
when they do it’s to assist folks with sure kinds
of anaemia and for men who don’t produce sufficient natural testosterone.
The results of the drugs shall be enhanced when mixed
with a nutritious diet. Anavar is a very fashionable drug amongst
gym-goers, because it’s one of the most secure anabolic steroids and comes with minimal side effects.
The drug far surpasses conventional testosterone within the physique, which makes it simpler to build and maintain onto muscle while getting lean.
That being said, 9/10 instances, these Steroids are going to be used in a fats loss section seeing as Steroid customers will go for different injectables to try to
enhance lean muscle mass. Nonetheless, like all steroids,
Anavar does carry some potential dangers and unwanted effects, significantly when used
in excessive doses or for extended periods of time. These can include liver toxicity,
cardiovascular issues, and hormonal imbalances.
It is subsequently essential to use Anavar responsibly and under the guidance of a
healthcare professional.
Nonetheless, stacking Anavar with other anabolic steroids can improve a user’s outcomes.
The optimal every day dosage of Anavar varies depending on several elements, such
as your gender, body weight, experience with steroids,
and desired outcomes. Anavar ought to be taken after consultation with a healthcare specialist, particularly regarding
its dosage. The perfect dosage of Anavar 20 mg varies primarily based on particular person goals,
gender, and experience with performance-enhancing medication. However,
typically, the patient is prescribed 2 to four tablets every day.
As a result, the risk is even larger when attempting
to acquire this steroid as dealers often cut the dose with out you understanding, or sell you
fillers to increase their revenue margins. ALL anabolic steroids will shut down testosterone levels to different extents.
How much you’ll be shut you down will range, depending on which steroid you take.
#4 Toxicity – As Anavar is consumed orally it must cross through the liver, and
although Anavar is considered a gentle steroid you must be careful.
There ought to be no alcohol consumed whilst taking
the drug and it’s suggested to seek the advice of your doctor if you’re
taking any present drugs. As A Outcome Of
anavar can build muscle and reduce body fat simulatenously, whilst having minimal side effects; it’s straightforward to understand why health club rats are popping
var tablets like they’re sweet.
And getting the best dose when you’re bulking is necessary, particularly if you’re making an attempt to minimize unfavorable side effects, or stack with your current weight in mind.
For one factor, the demand for black-market Anavar in capsule type will doubtless increase.
This will create a distinct segment for even more
underground suppliers, however may lead to poor-quality drugs and a threat of contaminated
substances. The liquid form of Anavar was
first produced in 1964 as a treatment for muscle wasting in older and chronically sick adults.
The consequence is retaining muscle mass whereas cutting
fats by preventing the body from going right into a catabolic state where muscle tissue is misplaced,
as is when nitrogen stability turns into negative18.
Oxandrolone was little doubt determined to be a mild
anabolic steroid method back then, which made it possible to be tolerated by feminine and child patients10.
Anavar is a fast-acting steroid derived from DHT (dihydrotestosterone)4 with a half-life of 8 to 10 hours.
The medically prescribed dosage for Anavar
is 2.5 mg to 20 mg, given in 2 to 4 divided doses.
This dosage is extraordinarily low compared to what’s obtainable in the recreational world.
Lifters will use 10mg per day upwards of 100mg for the upper elite, whereas some bodybuilders can take up to 120mg of Anavar per day.
Anvarol works by helping your body to supply extra phosphocreatine.
Phosphocreatine is necessary for producing vitality throughout
short, intense bursts of exercise, similar to lifting weights.
Anvarol can help you to train more durable and longer than before, resulting in amplified muscle growth and faster features in power and
size. Males are usually more sturdy when it comes to steroids
than ladies; the rationale for this is that Androgenic side effects are simply not as unhealthy on males
as on females.
This results in infected cytokines, a bunch of proteins produced in the kidneys, and markers of increased stress.
The second group, which took a better dose of 40
mg, skilled a 33% lower in HDL while elevating LDL
levels by roughly 30%. Men who acquired eighty mg of Anavar per day skilled a 50%
decline in HDL levels. Nevertheless, it is not
merely strength and endurance athletes that will profit from Anavar, with some
sprinters, swimmers, and boxers also using Anavar to gain a aggressive edge.
Ready for this to naturally occur just isn’t an possibility
as a result of low testosterone is significantly debilitating.
Anavar is far from probably the most suppressive steroid we will
use, however it’ll still have some impression on your regular testosterone production32.
Side results brought on by rising estrogen ranges come about when a
steroid causes the conversion of testosterone into estrogen (also known as aromatization).
One of probably the most appealing things about Anavar is that it does NOT aromatize and, subsequently,
does not trigger estrogenic side effects. And identical to the
constructive outcomes, the standard of your Anavar can play a BIG half in the varieties and severity of unwanted
facet effects. This is one extra reason we must always keep
away from poor-quality Oxandrolone on the black market by solely
shopping for from dependable suppliers. A standard PCT cycle will typically not restore testosterone
ranges following Trenbolone use, and longer-term TRT may be required.
References:
best Steroids for Athletes
Anvarol increases your ATP ranges, supplying you with extra energy and making your
workouts more effective. There isn’t much difference in Anavar dosage for bodybuilding purposes
whether you’re a person or lady. It is essential
for ladies to make use of Anavar with warning because of the potential for virilization, which is
the development of male-like characteristics. Many men choose to make use of Anavar as a end result of it is
an efficient method to construct muscle and cut weight fast.
Moreover, Anavar just isn’t aromatized by the physique, so it won’t convert into
estrogen. This makes it a good selection for men who are concerned
in regards to the development of man breasts (gynecomastia).
Anavar may be stacked with different steroids – however
it isn’t necessary.
User narratives and photographic evidence typically reveal
a notable transformation in people who’ve used these tablets
as a part of their health technique. Anavar is primarily
taken orally, a key distinction from many injectable anabolic steroids.
Its C17α-alkylation allows effective systemic absorption by way of oral tablets,
sometimes available in 2.5 mg, 5 mg, or 10 mg doses for exact changes.
Due to its brief half-life, customers often cut up daily doses to
maintain stable blood ranges. One of the most regarding unwanted effects for girls
is virilization, the place they begin to develop male characteristics as a end result of elevated
testosterone levels.
Relying on how you react some individuals have taken doses as a lot as 100mg every day,
although it isn’t really helpful as a result of put on and tear on the liver.
Some males also discover that Anavar helps to extend strength and endurance, which may be helpful
for athletes and bodybuilders. Overall, Anavar is a popular alternative for males who
need to enhance their physiques without placing their well being at
risk. As Quickly As an optimum dose is established, think about sticking
with it for the size of the Oxandrolone cycle, which is typically 6-8
weeks. If all goes nicely, there should be no reason to extend the dose additional, as results don’t
necessarily improve with larger doses, but
health risks would possibly.
Enhanced muscular definition is feasible after a single Anavar cycle
for ladies, even at decrease doses of 10mg. Winstrol is far harsher on the liver compared to
Anavar, even though they’re each oral steroids.
This facet impact alone might be enough for many ladies to steer the choice to Anavar over Winstrol.
Unlike another popular dihydrotestosterone derived anabolic steroid in Anadrol,
Anavar is what we’d name a rather facet effect friendly anabolic
steroid. Aspect results are actually potential, but for the wholesome adult they are often minimized.
In truth, with accountable use, many will
discover they experience no negative results at all.
In order to know the unwanted side effects of Anavar, we have damaged them down into their separate categories with all of the related data you’ll want.
Anavar is tremendously appreciated by many athletes for a few
specific causes. This steroid will enhance power; the
whole enhance is not going to be as significant as steroids
like Dianabol and nowhere near the extent of Halotestin, but it will be notable.
Power is among the main factors of successful athleticism because
it interprets into velocity and energy.
We advocate that if you resolve to make use of it, you should persist with the dosage.
Do not, for any reason, enhance your dosage.Anvarol vs Anavar, which do we recommend?
If you want fast results then Anavar may be best but should you want a extra healthy, efficient
result with no unwanted facet effects then Anvarol
could be the answer.
As with all such selections, it’s critical to
take gradual steps, adjusting primarily based on personal
expertise quite than dashing to achieve optimum dosage rapidly.
Bear In Mind, the target is not only about gaining muscles,
but also guaranteeing holistic wellness. Whilst indications point
in course of the Oxandrolone tablets being gentle on the body, it’s essential to recollect everybody is unique.
Beginning gradual gives time to observe and perceive how the physique is responding, as effects can differ across people and
gender.
This is indicative of the product being underdosed,
as 20 mg is more than adequate to expertise significant changes in body composition. A
common scam we have been made aware of is sellers labeling products
as Anavar, but the uncooked ingredient is Dianabol. Dianabol is a really
cheap oral to produce; thus, by deceiving individuals on this means, sellers can dramatically increase their revenue
margin. Our feminine patients have reported feeling depressed and have skilled low libido upon cycle cessation.
Its generic name is oxandrolone, and it was initially developed to assist individuals recover from weight reduction because of surgical procedure, infections,
or major burns. Not Like another steroids, Anavar steroid is known for its ability to help construct lean muscle with out causing a lot of water
retention. This makes it well-liked not just for medical use but additionally
amongst athletes and bodybuilders seeking to enhance their performance and appearance.
World Pharma’s Anavar 20mg (Oxandrolone) is a
highly regarded anabolic steroid recognized for its effectiveness in selling lean muscle positive aspects and fats loss.
Recognized as one of many safest oral steroids, Anavar is appropriate for both men and women.
Nevertheless, people in these nations need to be cautious to not abuse this steroid, as like with any drug – should you abuse it,
you’re in bother. Nevertheless, contrary to
anavar, wild yam root HAS proven to increase HDL levels of cholesterol and improve cardiovascular health.
Studies have proven that taking 5.6g of BCAAs post-workout can stimulate protein synthesis by 22% (3).
Nonetheless, anvarol accommodates a fraction of this, with a baby dose
of 75mg per pill. Even if you took the whole bottle of anvarol you’d simply get enough to stimulate this very modest increase in protein synthesis.
References:
side effects of steroids for muscle building (Shona)
This is helpful for bodybuilders who are in search
of maximum mass. Such muscle fullness, mixed with Anavar’s diuretic properties, can lead to more
prominent vascularity. We have found that DHT-related side effects are largely decided by genetics.
Thus, some people could experience vital hair loss from a low
dose of Anavar. Whereas others might expertise no hair loss
whereas taking excessive doses of trenbolone.
The major ingredient, oxandrolone, helps muscle development and boosts energy.
A typical PCT protocol after an Anavar cycle may contain the utilization of selective estrogen receptor modulators
(SERMs) such as tamoxifen or clomiphene. These drugs work by stimulating
the body’s pure manufacturing of luteinizing hormone (LH) and follicle-stimulating hormone (FSH),
which in turn promote the manufacturing of endogenous testosterone.
The duration and dosage of the PCT will differ based mostly on the length and dosage of
the Anavar cycle, as well as particular person factors.
Nonetheless, when you do go down this route don’t buy from
corporations with poorly designed websites or ones which don’t list their handle,
as you could get scammed. People additionally sell Anavar on the
black market, which is the place most people get it from.
Oxandrolone is used to assist you regain weight lost after surgical procedure, extreme trauma, or chronic infections.
Oxandrolone is also utilized in individuals who can not achieve or maintain a
healthy weight for unknown medical reasons.
To help you maintain your positive aspects and make sure you’re caring for your well being, our
consultants will help you choose the most effective oral
steroid doses and post-cycle treatments. We are licensed and lively IFBB
professionals, we are also a reputable online anabolic steroid source with over ten years of expertise on this subject.
Our major objective is to help you obtain your muscle-building,
bulking or weight reduction targets safely.
When that is sneakily accomplished, men will discover extra bloating and water retention, along with
distinctive muscle and energy gains. Nevertheless, Anavar causes
more gentle gains in size, with vital fats loss and
no water retention. Males use it to build vital amounts of lean muscle and
burn fats (2), without experiencing harsh unwanted effects (which are very common with different
anabolic steroids). Hi-Tech Pharmaceuticals’ Anavar
contains a strong formula that begins with 4-Androstenolone (4-Andro).
Anavar – chemical name Oxandrolone, is doubtless considered one of the hottest oral steroids and most generally used anabolic steroids right now
and this has been the case of decades. With an all round good status for lean bulking
cycles, chopping and use in low dosages for girls, one can understand
why its so well-liked in the steroid utilizing world. In Accordance to
data from US-based sports drugs publications, Anavar is among the few anabolic steroids extensively tolerated
by girls because of its low androgenic activity. Feminine users often make
the most of doses as little as 5–10 mg daily to achieve a lean, sculpted physique without vital
danger of masculinizing side effects. Men utilizing Anavar may experience a quantity of particular unwanted side effects associated to their hormonal stability and reproductive health.
One of the main considerations of Anavar for males is the suppression of natural testosterone manufacturing.
Most individuals would find that the price of pharmaceutical-grade Anavar would just not
be worth it, as it’s significantly more expensive than most
different, extra widely out there steroids. Anavar have to be sourced carefully to ensure you get what you want – accurately dosed and
high-purity Oxandrolone (preferably pharmaceutical-grade).
Availability and ease of access, legal conditions, and pricing of Oxandrolone will differ across different
components of the world. Positive reviewers will state that Anavar is essentially the most well-tolerated
steroid they’ve used. Still, it’s important to examine out what dosage
they’ve used so you’ll find a way to determine how the dose
would possibly affect your outcomes and (lack of) unwanted
side effects. This allows us to realize insight into how totally
different individuals expertise Anavar.
When seeking to buy this supplement, you are not more doubtless to discover
it listed or labelled utilizing that name on any current formulations.
Regardless Of this, the name Anavar remains to be generally used
to describe this compound. “I even have placed about 5 orders with ROIDRX and all have gone perfectly. I often get my order in just in the future and its always prime quality.” “Discovered roidrx very helpful…their service was promt and product wonderful…might be doin enterprise with them for alongside time.” “Simply the best products and service. Tri-tren is by far my favourite. tren A and tren e is gave me finest outcome…”
Almost all steroid sources will offer some brand of Anavar to their clients.
You can find Anavar on the market by native fitness center dealers in the majority of countries
where steroid use is clear. Local fitness center sellers are
sometimes priced greater than other avenues of sale,
similar to On-line. Gym sellers will supply fewer brands than on-line suppliers, general
holding less stock. This means your choices are reduced in comparability with buying Anavar on-line or when looking
for Anavar on the market on-line. There can be the added risk of
not being nameless or having any layer of anonymity if you
buy Anavar in real life by a fitness center source. Merely, you don’t
know whom this particular person is and in the United States the DEA have been recognized to sell anabolic steroids to individuals
operating sting operations the place authorized.
The greater your dosage, the larger your danger
of opposed well being effects. Anavar (oxandrolone) is an oral anabolic steroid created
in 1962 to promote lean muscle mass in those affected by muscle-wasting
circumstances. The different primary goal when formulating Anavar was to create a gentle drug
with few side effects so women and kids may safely take it.
These supplements are designed to increase protein synthesis,
boost libido, scale back estrogen levels, and aid fats loss.
They also help to keep your testosterone ranges high, which
is a necessary issue for maximizing lean muscle development and
stopping muscle loss through the chopping cycle.
If you are looking for steroids for sale, then you should know that it could enhance muscle mass and power, enhance endurance
and reduce physique fat.
If you take Anavar for building muscle, it’s best to stack it with other dietary supplements.
Nevertheless, talk about the side effects and potential interactions at length with your
doctor to be secure. Pharmaqo is a leading steroid model, offering high quality
merchandise to gym fanatics for years. Earlier Than using
oxandrolone, inform your doctor or pharmacist if you are allergic
to it; or in case you have another allergy symptoms.
Children who use this medication could have to examine their X-ray bone growth rate each few months.
You mustn’t use this medication when you have breast or female cancer, prostate most cancers,
kidney problems, or high blood calcium ranges (hypercalcemia).
This Oral Steroid on the market can additionally be used to deal with bone ache caused by osteoporosis and other circumstances as prescribed by
your doctor. ● IT IS PSYCHOLOGICALLY EASIER TO ADMINISTER Starting with steroid pills is extra practical.
For example, nothing is stopping sellers from spiking sure
steroids they promote, as they aren’t regulated
and generally even produced in their basement. Additionally,
it is essential to prioritize correct vitamin, common exercise, and adequate relaxation during
the cycle to optimize results and minimize potential
risks. Combining Anavar with a balanced food plan and
a suitable training program can yield optimistic effects on muscle definition, power,
and general physique. I am a muscular guy with
much attention and recognition for my physique. I started with very little and always put 110%
into the gym to get to where I am now. From anabolic steroids to SARMs to peptides
and ancillary medicine, I’ve carried out it at some point in my life, and
I can relate.
References:
why is Steroid use among Athletes dangerous to their health (http://www.pharmalinkin.com)
Anavar is better often identified as Oxandrolone
which is a steroid derived from DHT with extremely anabolic functionality.
Men generally that want to go this route should purchase
more because the physiology is totally different they usually require a
bigger dose, often above 10mg that girls require. Are you contemplating
purchasing Clenbuterol in Mexico but not sure of the cost?
The product provides men and women with the flexibility
to expertise fast weight loss. Enhanced fat burn throughout coaching offers people with the means to
shed the additional kilos. Anabolic steroids could be detected in drug exams for several weeks or months after use.
Testing strategies vary but mostly involve analyzing urine or blood samples.
On the flip side, it’s crucial to think about the monetary dedication required to maintain a long-term Anavar routine.
It’s important to finances for ongoing treatment prices and to plan for
potential unwanted facet effects which will require extra medical therapy.
When it comes to determining the value of Anavar 50mg tablets, model
reputation plays a big function within the overall value evaluation.
Dr. O’Connor has over 20 years of expertise treating women and
men with a historical past of anabolic steroid,
SARM, and PED use. He has been a board-certified MD
since 2005 and offers guidance on harm reduction methodologies.
In this instance, customers will also expertise water retention and bloating, which Anavar does not trigger, plus heightened anabolic effects.
We have found that valerian root supplements may be efficient for gentle insomnia,
lowering the time taken to fall asleep and the quality of
sleep (36, 37). In one research, members reached sleep 36% sooner
after a single dose of valerian (38). We find that
if junk foods are consumed during a cycle, sodium levels will rise, inflicting water retention. This can inhibit Anavar’s diuretic effects, causing the muscle tissue to seem more and more
smooth and scale back muscle definition, striations,
and vascularity.
Crazy Bulk’s formulas are supported by scientific research
and are safe for women and men to make use of. Alternatively,
they may decide to stack the above steroids at
the aspect of Anavar. We have found Olympus
Men to be probably the most cost-effective supplier, with remedies starting from $148 to $200 per 30 days.
Nonetheless, your healthcare provider could have more information regarding specific packages
obtainable in your space.
The half-life of Anavar presents 9 hours and serious bodybuilders have to take twice the dosage to achieve the expected expertise.
The product seems to current a less potent substance than the available alternate options and focus totally on fast weight administration. Professionals really helpful that critical bodybuilders
use the product with added testosterone-induced steroids as
properly. When it involves the worth proposition of Anavar 50mg tablets, one of many key elements to contemplate is
its value point.
Conversely, if the provision is proscribed or there is a high
demand, the price may behigher. Components corresponding to authorized restrictions, regulatory controls, and market developments can affect the supply and demand dynamics, thereby affecting the value of
Anavar. Skilled steering, such as consulting with a
healthcare supplier or health professional, can further optimize your outcomes while mitigating potential risks.
The underground market is rife with counterfeit or substandard products, offering
no assure of purity or efficiency. Customers opting for these dubious substitutes might not only experience disappointing results but can also expose themselves to harmful unwanted aspect
effects as a outcome of impurities and contaminants present in the product.
Nonetheless, its adoption outdoors the medical sphere has
been equally spectacular. Athletes and bodybuilders have
recognized Anavar as a powerful device for sculpting their physiques,
enhancing muscle definition, bolstering energy, and
elevating general physical efficiency. The twin nature of Anavar, with its capability to bridge the divide between medical necessity and athletic ambition,
underscores its significance in the modern world of
prescribed drugs and sports activities science. The same could be mentioned with
Anavar or any other efficiency enhancing drug, there are benefits but as we’ve mentioned
there are risks too.
Both trenbolone and Winstrol do not aromatize,
so water retention won’t be a problem, leading to a defined
and dried-out physique instead, with enhanced vascularity.
Thus, high calories mixed with the estrogenic nature of testosterone and Anadrol will
trigger significant water retention, even with trenbolone’s diuretic properties.
We have discovered the risk of gynecomastia to be excessive with
this stack, with estrogen levels rising in the presence of Anadrol and testosterone.
As A Substitute, Anadrol directly stimulates estrogen receptors; thus,
a SERM might help to forestall gynecomastia from Anadrol (albeit at the threat of
exacerbating progesterone levels within the presence of trenbolone).
Anavar (Oxandrolone) can be a useful device in your bodybuilding journey, providing unique advantages that can improve your efficiency and physique.
By understanding the pricing, dosage recommendations, and potential
unwanted effects, you can make informed decisions when incorporating this steroid into your regimen. When it involves utilizing Anavar in bodybuilding, understanding the
suitable dosage is essential for attaining desired outcomes
whereas minimizing potential unwanted effects. This table presents dosage suggestions for Oxandrolone
starting from newbies to intermediate and superior users. By following these tips and consulting with a
healthcare professional, you can make knowledgeable choices about your steroid dosage.
In our experience, bodybuilders have an increased
threat of nephrotoxicity, with a number of of our sufferers displaying high
creatinine levels from renal perform exams. Leal Herlitz, MD, examined
the kidney function of 10 bodybuilders who had utilized steroids
long-term.
Stacking Deca Durabolin with an androgenic steroid
such as Anadrol, testosterone, or trenbolone can mitigate
low NO levels. Deca Durabolin’s weak androgenic nature, when combined with high prolactin ranges, causes instances of
erectile dysfunction. When androgen levels are inadequate, nitric oxide (NO) concentrations decrease.
Enough NO manufacturing is crucial for the availability of blood to penile tissue.
The Portuguese doping lab Laboratorio de Analises de Dopagem
performed the peer-reviwed and double blind study giving
the patients 300mg of caffeine mixed with Oxandrolone. The researches witnessed a rise in plasma concentrations in the Oxandrolone +
Caffeine group when compared with the Oxandrolone alone group.
Reliable suppliers typically share Certificates of Evaluation (COAs) or independent lab
results proving the product accommodates real Oxandrolone at the marketed dosage.
Look for well-reviewed and established manufacturers,
also recognized as UGLs (Underground Labs). Well-liked names like Pharmaqo, Alpha Pharma,
Dragon Pharma, and Meditech tend to supply more reliable products.
Shopping For poor-quality Anavar isn’t just a waste of money—it can compromise your well being and your results.
It also can affect your blood ‘thickness’, by growing your pink blood cell depend.
Nevertheless, its use exterior of medical supervision can result
in significant well being risks and unwanted side effects, including
liver toxicity, cardiovascular issues, and hormonal imbalances.
It displays lower androgenic properties, decreasing the danger of virilization unwanted effects.
Nonetheless, it’s essential to use Anavar responsibly and
follow correct dosage guidelines to minimize the potential
for opposed effects. Lastly, individual components similar to genetics,
metabolism, and hormone ranges affect how Anavar impacts each
person. Whereas some users may experience vital gains in strength
and muscle mass inside the first two weeks, others might notice extra gradual modifications.
References:
steroid side effects for women (Allison)
Anavar, very like Dianabol is definitely a very highly effective anabolic steroid,
but it does have the facility to produce androgenic unwanted effects.
Extra customers than not still undergo from oily pores and skin, breakouts on the
again and shoulders in addition to deepening of the voice and an increase in body
hair development. Anavar binds to the Androgen Receptors (ARs) of the muscle cells and stimulates protein synthesis, which will increase
muscle progress, lean body mass, and bone mineral density.
To obtain optimal outcomes, the timing of Anavar administration is crucial.
Many athletes and bodybuilders prefer splitting the day
by day dosage into two equal elements with morning and night administration. This helps keep regular blood levels of the drug
all through the day, maximizing its effectiveness.
Some people may naturally have a faster metabolic rate or be extra
aware of steroids, leading to faster outcomes.
Another factor that influences the onset of action is the user’s
total well being and way of life selections. People who comply with a
nutritious diet, interact in common exercise, and get ample relaxation and
recovery could expertise quicker outcomes in comparison with those that neglect these components.
Anavar, a potent steroid extensively used within the medical
field, is known for its rapid results. Understanding the onset
of action is crucial for users looking for immediate results.
This section will explain when users can anticipate to begin experiencing the effects of Anavar and focus
on the components that will influence the onset of motion.
Analysis from 2012 saw severely burned youngsters experience an enchancment in muscle power that lasted for
as much as five years post-burn (7). One Other research from 2007 revealed that “muscle power considerably increased” in burn victims when oxandrolone and exercise were mixed (8).
If you’re looking to obtain a leaner physique, then Anavar may be an effective
fats loss software.
Anavar helps to offset this by serving to to preserve muscle
tissue whereas the bodybuilder is cutting weight.
In addition, Anavar helps to extend strength and stamina, which may be beneficial through the grueling process of chopping weight.
Simply put, gaining muscle can provide a aggressive edge in any bodily exercise.
However, you will want to remember that food regimen,
train, and supplements play a critical role in successful muscle gain. With Out a proper food regimen and train regime, it is very difficult to add significant quantities of muscle mass.
Doctors discovered his liver was severely broken, and he died within two days of reporting for
treatment as a result of severity of injuries to his liver.
Anavar could assist with fat loss but just isn’t a “miracle” drug that will trigger you to lose
large amounts of body fat shortly. Be positive to speak to your physician before starting any new supplement regime, especially when you have
pre-existing well being situations or are taking other medications.
It also increases red blood cell manufacturing by as a lot as 50 percent which
permits Anavar users to perform extra reps throughout exercises
– ultimately leading to leaner muscle tissue.
Anavar is an anabolic steroid that was by no means really developed for use
as a remedy for obesity. That stated, we all know it could
result in some fats loss in both men and women.
If you experience any changes in your skin color while taking Anavar, you want to report
them to your doctor. In most instances, the discoloration will resolve on its own when you cease taking the treatment.
For now, plainly Anavar could additionally be a promising option for many who want to improve their stamina.
One potential benefit of Anavar is that it may help to increase stamina.
This means that your physique will have the power to burn extra calories, even when you’re at relaxation. Thus,
it is unlikely that someone could be examined for steroids
within the military, particularly if they are quiet
about their use.
Anavar, also called Oxandrolone, is a well-liked
steroid used for chopping cycles. It is thought for its gentle androgenic effects and is commonly used by each men and women. One of the commonest questions folks have
about Anavar is how long it takes to work.
In uncommon circumstances or when users have been on cycle for extended periods,
people can be shut down permanently or suffer from low testosterone levels for
many years. When run alone cycles will sometimes be four
– 6 weeks in size in doses starting from
30mg day by day to 50mg on the higher finish. Depending on the way you react some individuals have taken doses up to 100mg every day, though it isn’t recommended because of
the wear and tear on the liver. Tablet formed steroids like Anavar are
very fashionable as a outcome of they can be consumed orally
and no injections are wanted. For those who don’t know, the main two attributes of anavar is to burn fats and improve energy.
Anavar is commonly used by bodybuilders and athletes to boost their performance and enhance their physique.
Thirty-two wholesome adult males aged 60–87 have been randomized to receive 20 mg of Anavar per
day or a placebo for 12 weeks. The results confirmed that Anavar elevated
lean physique mass by a mean of seven kilos and improved maximal power by 7.5%.
Men using Anavar could experience several particular unwanted facet effects associated
to their hormonal balance and reproductive well being.
One of the leading concerns of Anavar for men is the suppression of natural
testosterone manufacturing.
References:
Steroids.com Review
Several steroids are additionally accredited by the FDA, but they remain illegal at present in most nations.
At Present, steroid use solely becomes legal when prescribed by
a medical doctor for underlying health issues (11).
The most secure oral anabolic steroid in our testing is testosterone undecanoate.
Nonetheless, Anavar and Primobolan are also very mild
compounds with few unwanted effects. Moreover, these were bodybuilders
taking steroids at a time when no one had established their security.
Right Now, bodybuilders are capable of mitigate the dangers as a result
of higher information of the compounds and cautious dosing.
In bodybuilding, we see testosterone predominantly used in bulking cycles to add massive amounts
of muscle and power.
Due to its sedative and GABA-boosting properties, it can additionally be used to scale
back anxiousness and despair (40). Thus, it is unlikely that somebody
would be tested for steroids within the army, especially if they’re quiet about their use.
However, they can test for steroids, particularly in instances where they are known to be rife in a particular unit or if there’s another excuse to suspect
someone of using them. Clenbuterol works by stimulating thermogenesis,
inflicting an increase in body temperature, and elevating the metabolism.
In flip, this causes them to lash out at anything and anyone and might
finally result in violence. This is known as “roid rage” and occurs most of the time to folks abusing steroids.
Sure, it’s at all times a good idea to talk to your physician before
using any new complement or drug, including Anavar. Your doctor
may help you perceive the potential dangers and advantages, in addition to any potential interactions
with different medications you might be taking. The legality of purchasing Anavar varies relying on your location and the particular
laws in your nation. In some international locations, Anavar could additionally
be obtainable only with a prescription from a licensed healthcare
skilled.
Beforehand, we cited a research that acknowledged men taking 20 mg a day for 12 weeks experienced a 45%
lower in testosterone ranges. This was an excessive cycle length,
with a standard cycle length of 6–8 weeks for males.
From this study, we will conclude that natural testosterone manufacturing is more probably to remain fairly high
if a average dose or cycle is performed.
Anavar impacts copy by doubtlessly lowering sperm rely
or disrupting hormonal balance. It Is essential to bear in mind these dangers and
consult a healthcare professional for guidance. Moreover, natural dietary supplements corresponding to
fenugreek and ashwagandha have shown promise in naturally boosting testosterone ranges,
promoting muscle acquire, and enhancing general performance.
These botanical ingredients provide a safer, legally
compliant alternative to synthetic anabolic agents.
So, while the thought of achieving spectacular positive aspects in power and muscle mass
via steroid use may be tempting, it’s essential to weigh the risks against the rewards.
Crazybulk is a good firm that sells legal steroids that are secure and efficient.
If you’re on the lookout for a secure, authorized different
to steroids that delivers actual results, Anvarol
is a perfect choice. Nonetheless, because of its potential for abuse, it is classified as a controlled substance in some nations.
A steroid drug for weight loss that was first made available by G.D Searle & Co.
again in 1962, Anavar is an orally-administered medicine that is
carefully related to testosterone. Anvarol
isn’t a steroid and doesn’t contain any illegal or doubtlessly harmful ingredients.
Anavar is extremely reviewed amongst othe efficiency enhancing
supplements. This is likely certainly one of the commonest anabolic steroids used to combat muscle losing
ailments and in some circumstances even osteoporosis, while used
to advertise lean tissue gains. Anavar’s results, nonetheless,
prolong past medical purposes, making it a favored substance in the bodybuilding neighborhood.
Its attraction lies in its decrease androgenic effects in comparability with other anabolic steroids, which reduces the risk
of certain unwanted effects and attracts both female and male users.
If injected incorrectly, any steroid or treatment may be harmful (or fatal).
From 2001 to 2011, testosterone prescriptions have tripled (1), indicating a present low testosterone epidemic.
The army takes substance abuse very critically and only sends
soldiers who are both mentally and bodily wholesome into battle.
If somebody is discovered utilizing steroids they could probably be
disqualified from serving within the army.
But if you completely want to use Anavar, then you
should be aware of the potential dangers. Additionally, if you’re a man with low testosterone levels, Anavar is usually a
good option. This side effect is commonest in teenage boys and young men, as their bodies are
nonetheless creating and are more sensitive to the results of steroids.
Creatine is renowned for enhancing energy production, while whey protein provides essential amino acids very important for muscle synthesis.
In addition, when you’re fighting steroid dependency,
counseling providers and assist groups provide important sources for recovery and more healthy life-style choices.
It’s advisable to hunt in depth assist from respectable health applications and nutritionists,
making certain your efficiency enhancement methods comply with authorized standards.
Understanding these penalties and the complexities of enforcement is essential.
International variations necessitate careful navigation of authorized necessities to keep away from unintended violations.
References:
what’s In Steroids
70918248
References:
testosterone schedule drug (Nicolas)
70918248
References:
steroids before and After 3 months, e-hp.info,
70918248
References:
https://www.belkataherkhani.ir/?p=1167
70918248
References:
Steroid Websites (https://bmrbl.teamsnapsites.com/2023/04/26/hello-world/)
70918248
References:
steroid fat burner (https://multistyle.work/helping-companies-in-their-green-transition-3/)
70918248
References:
http://www.evahoudova.com/index.php?article3/renee-pietrafesa-dirigeante-dorchestre
70918248
References:
best legal steroids reviews (https://bayridgehoa.com/2023/07/26/bay-ridge-community-club-lot-map/)
70918248
References:
none – https://ailcare.com/heart-is-courageous/ –