Imagine falling dramatically ill from an autoimmune condition that causes your body to attack your brain, only for everyone around you to assume you’re going mad.
“The doctors just kept telling me I was having this breakdown due to the pandemic,” Ms Hawkins says.

It would take almost six months for Ms Hawkins, 35, to find a neurologist who knew what was really going on and diagnose her mystery illness – autoimmune encephalitis.
The rare condition is often described as making patients feel like their brain is on fire.
It is the subject of Netflix documentary by the same name, Brain on Fire, based on the true story of former New York Post reporter Susannah Cahalan who almost ended up in a psychiatric ward when doctors believed she had schizophrenia.
‘I couldn’t taste or smell’
Ms Hawkins remembers the day her life began to suddenly fall apart with the same condition.
It was April Fools’ Day last year.
The family was living in an RV at the time in Yamba, on the northern NSW coast, having spent the past 18 months travelling around Australia.
She had woken up in the morning dizzy with vertigo, something that had never happened to her before.
Ms Hawkins, who was then studying for her nursing degree, said the thought crossed her mind that she might be having a stroke.
But it was later that day, when she was eating her husband’s favourite spicy soup dish, that she knew something was really wrong.
“When I’m eating this dish I usually carry on like an idiot, grunting at how spicy he makes it and blowing my nose as the heat takes over. To my surprise, half-way through the dish I realised I couldn’t taste or smell the soup,” Ms Hawkins said.
“I panicked and told my husband, who said, ‘Oh no, you have COVID’.”

Ms Hawkins went to the doctor, who ordered a blood test to check for any viruses and prescribed some medication for the vertigo.
Then she went into the pharmacy to buy the medicine – and it was there her reality began to warp.
Without being aware of it, Ms Hawkins was acting very aggressively towards the pharmacist, swearing and spitting.
“He explained my behaviour was not acceptable… I was confused and scared and knew deep down something was seriously wrong with me,” Ms Hawkins said.
Ms Hawkins rushed back to the doctor’s office.
“I was taken into the examination room and it was discovered I had lost vision in my left eye. I was extremely confused and failed the neurological exams,” she said.
“The doctor rang my husband and explained I needed to go straight to hospital.”
At the hospital, Ms Hawkins couldn’t remember her date of birth, couldn’t sign her name and hardly knew where she was.
But a CT scan showed up nothing unusual and she was discharged the next day with a referral for a mental health doctor.
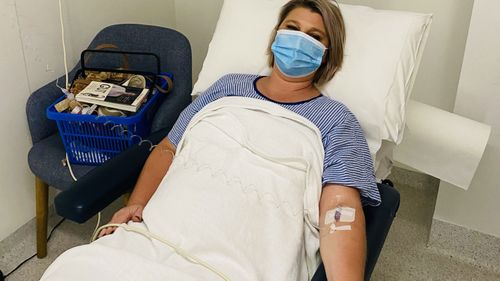
The next day her husband took Ms Hawkins to a different hospital, where she passed the neurological examination and was discharged, with doctors suggesting she may have anxiety issues due to the COVID-19 pandemic.
“All blood tests and COVID testing had returned normal. The doctors could not find anything wrong with me,” she said.
What followed was weeks of agony where Ms Hawkins’ condition continued to deteriorate without explanation.
“I was slowly losing the ability to function. I would slur my words and stutter. My head felt like it was being suctioned from the edges of my brain. The left side of my body had also lost function,” she said.
“I could not remember anything… basic objects no longer had names.
“I remember my daughter asking me to brush her hair. I vividly remember saying, ‘If you can show me what a brush is, I can figure out how to use it’.”
In desperation, Ms Hawkins got a private referral to see a neurologist on the Gold Coast two weeks after she first fell ill.
She says the neurologist told her she had “some sort of inflammatory response in the brain” and would likely get better if she rested up at home.
A repeat MRI showed up nothing unusual.
The family decided to move to Bribie Island in Queensland to be nearer to family.

In May, Ms Hawkins said she did miraculously start to feel better.
“My speech and vision returned. My sense of taste and smell slowly came back. I could identify objects and use cutlery. I could wash and dress myself again.”
But after three weeks of respite, the symptoms returned.
“I was sleeping 15-19 hours a day. The spinning in my head was worse than ever. I felt like my brain was burning.”
Ms Hawkins said she was hearing voices in her head, having delusions and could not even recognise her own children.
“The scariest moment for me was when I did not recognise my children. I could not figure out who they belonged to. In my mind, I knew they did not belong to me and I thought, ‘what on Earth were these small humans doing in my house,'” she said.
In and out of doctors’ offices, it took until August for a breakthrough when she was referred to a leading Brisbane neurologist, Dr Stefan Blum, who specialises in complex cases.
Five days later she had her diagnosis.
How common is autoimmune encephalitis?
However, Dr Blum, who is also an associate professor at the University of Queensland, said much was still unknown about how common it is.
“There is a lot of new data that has come out since 2008, mostly relating to the antibodies that are causing this condition,” Dr Blum said.

“It was thought to be extremely rare and only seen in patients with cancers and now it is a bit more frequently diagnosed, even though we still don’t know a lot about this condition.”
Some triggers for the condition were obvious, such as a tumour, Dr Blum said.
Other potential triggers could be a virus or infection, but often the cause was never discovered at all, he said.
Dr Blum, who currently treats around 30-40 patients with autoimmune encephalitis, said it was relatively common for patients with the condition to come to the attention of a psychiatrist first.
Although increased awareness in recent years meant most psychiatrists were testing for, and therefore diagnosing, more cases of autoimmune encephalitis, it was still not known how many were being missed, Dr Blum said.
“Are there still a lot of people around who are not getting diagnosed? Probably. I can’t say for sure but it is certainly a probability,” he said.
“We are doing a study at the moment with the University of Queensland and a few other sites to answer precisely that question.
“How many patients in the psychiatric world do actually have autoimmune encephalitis?”
It builds on research which showed five of 113 patients admitted to hospital with a diagnosis of psychosis had antibodies and evidence of inflammation associated with autoimmune encephalitis.
Ms Hawkins said although she was initially thrilled to get her diagnosis, her recovery had been slow.
Inflammation in her brain has left her with some damage to her frontal lobe.
“I’m still not able to work and am on a lot of medication that I am slowing trying to wean off,” Ms Hawkins said.
“Autoimmune encephalitis is not something that you cure but I’m hoping that I will one day get to a point where I am in remission.”
Ms Hawkins said she was determined to speak out about her condition in the hope of reaching others who may be going undiagnosed or have loved ones who are.
Contact reporter Emily McPherson at emcpherson@nine.com.au
This content first appear on 9news
