California leaders are under fire over the state’s mixed messaging on how people with disabilities will be prioritized for the Covid-19 vaccine, a situation that advocates say has left millions of disabled and chronically ill residents in the lurch.
Last month the state’s governor, Gavin Newsom, abruptly announced California would diverge from national guidelines set by the Centers for Disease Control and Prevention by prioritizing age, rather than underlying risk, in deciding who would get the inoculation next, arguing it would “allow us to scale up much more quickly”.
The move, however, was fiercely criticized for leaving people with a range of physical and developmental disabilities and medical conditions confused about when their turn would come. Advocates called on the state to reprioritize high-risk Californians – including people with disabilities.
However, on Friday afternoon, officials changed course, announcing that people ages 16 to 64 with high-risk conditions including cancer, kidney disease, and weakened immune systems, as well as people with developmental disabilities, will have access to Covid-19 vaccines after 15 March, along with food workers and educators. Doctors can also offer the vaccine to high-risk people who do not fall into categories set by health officials.
But the month-long wait for clarity, combined with the vagueness about which disabled residents do and do not qualify under the new policy, have only deepened frustrations.
“This new policy is not enough,” said Charis Hill, 34, a disabled activist based in Sacramento who has an autoimmune disease and takes medications that suppress their immune system. “It almost feels like too little, too late.”
Andy Imparato, the executive director of Disability Rights California, said the Friday announcement “is a huge step forward”. Imparato has been attending meetings with the Community Vaccine advisory committee, a panel of experts and stakeholders, about the distribution plans. He said he’d like the state to continue developing strategies to quickly reach disabled adults living in group homes, and those who require in-home health care providers. And, he added, “If we can move the March 15 date up as vaccine supplies ramp up, that would be my preference.”
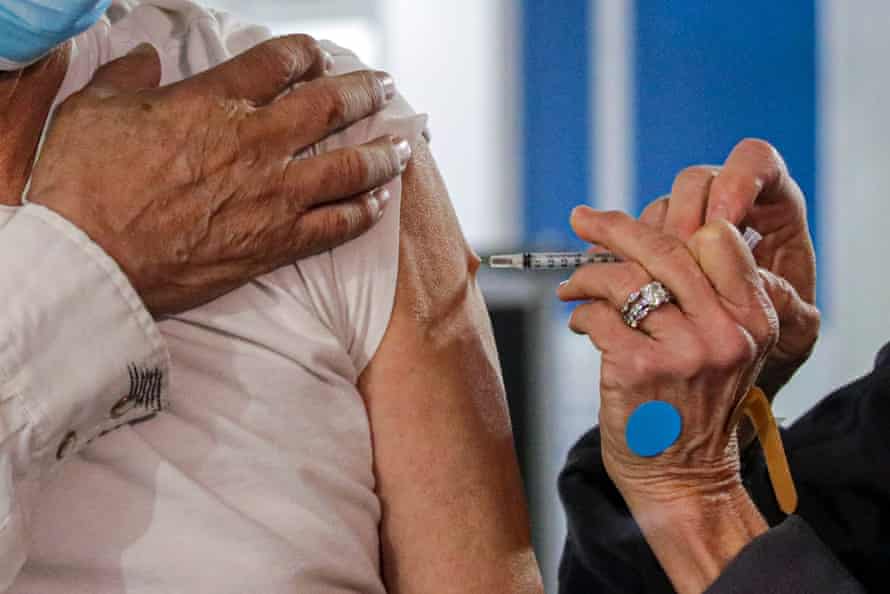
The new policy, which allows disabled young and middle-aged people to get vaccines from their medical provider or at mass vaccination clinics, leaves many unanswered questions. The state provided a list of “severe conditions” including cancer, chronic kidney disease, immune system vulnerability due to organ transplant, and pregnancy that qualify residents to access the inoculation.
Other disabled and chronically ill people will have to get approval from their doctors. “My disease group is not listed,” said Hill. “That immediately made me feel nauseous.”
Hill was worried about catching common viral infections even before the pandemic struck – for them a mild flu could turn into life-threatening pneumonia. For the past year, they have not left their house other than for unavoidable doctor’s appointments. “My in-person social interaction is almost all in the doctor’s office,” they said. “That’s the only time I touch a person, because it’s medically necessary.”
The state’s back-and-forth on how to distribute vaccinations came a year into a pandemic that has discriminately and disproportionately infected and killed disabled people, either because of their frequent exposure to caregivers and health workers or because of suppressed immune systems and other complications. Neither California, nor the US, has comprehensively tracked how many disabled residents have died of Covid-19. The UK’s Office for National Statistics (ONS) found that nearly six out of every 10 people who died of Covid-19 in England were disabled.
“The decision to not prioritize disabled and high-risk people is essentially a death sentence,” said Hill.
More so than physical isolation due to their inability to safely leave home, Hill said they have felt a sort of “social and cultural isolation, from just being continually left out of the conversation and left out of planning for public safety and public health”.
The vaccine distribution across the US has been slow, and at times faltering – due in part to the limited quantity of vaccines. As the Biden administration works to speed up the process, many residents have questioned why California is trailing behind states with fewer resources, including Utah, the Dakotas and West Virginia, in administering the doses it has been allocated.

Both Utah and South Dakota have prioritized some or all residents with high-risk conditions above the general public – and South Dakota has begun to give vaccines to people with high-risk medical conditions and disabled people living in group homes, alongside the elderly.
California is currently offering vaccines only to people who are 65 years or older, nursing home residents and workers in healthcare, education, child care, emergency services, agriculture, and food services.
Alice Wong, a disabled activist based in San Francisco who uses a ventilator and home care attendants full time, said she worries about the permanent consequences that the pandemic will have on Californians who have not been able to leave their homes, and have delayed medical care and treatments for fear of catching the virus. “Not having the vaccine is an existential threat,” she said. “It’s a form of violence against disabled people. It’s eugenics.”
Wong said she doesn’t understand why Newsom’s government could not deliver the vaccine both efficiently and equitably, given that officials had a year to plan and prepare for it. “It angers me that it had to get to this point,” she said.
The governor’s office did not directly respond to a request from the Guardian for a comment, nor did the state’s Covid-19 vaccine taskforce. In a press conference on Monday, Newsom said the state would “take care of the most vulnerable and people in the developmentally disabled community” but added that “whatever we do will not be enough until the [vaccine] supply is adequate”.
Kristen Lopez, a Los Angeles-based entertainment journalist in her 30s with brittle bone disease, said the state’s initial tiered vaccine policy was far from ideal, “but at least it was understandable in some way. There was at least a timeline,” said Lopez.
Her mother, who is Lopez’s in-home healthcare provider, was part of the first tier of care providers who qualified for the vaccine. “As she was saying, it doesn’t make sense that care providers are able to get it, but not all the vulnerable people they’re caring for are.”
“At this point,” Lopez added, “it all just seems arbitrary.”
This content first appear on the guardian
